Combating the opioid epidemic: From treatment to prevention
Opioids kill enough people each day to fill a midsize jet.
In the late 1990s, pain was identified as the fifth vital sign, and prescriptions for opioids skyrocketed. Fifty percent of those prescriptions were for management of chronic pain.
Dosages increased, and they were prescribed for longer periods of time, but an unfortunate fact remained: Long-term use of opioids is not an effective treatment for chronic pain. Even when taken as directed, increased usage leads to increased risk for addiction and overdose.
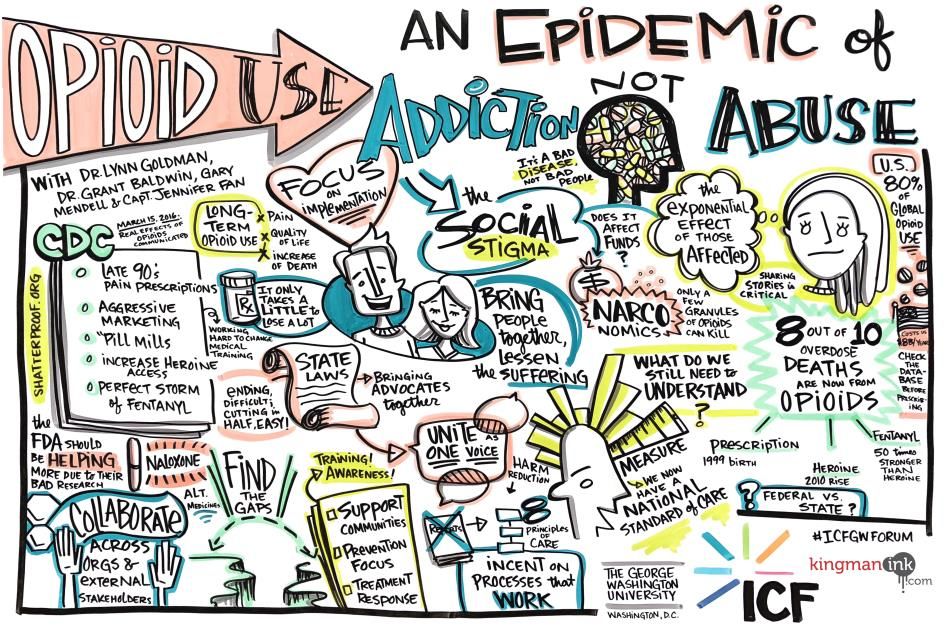
Dr. Grant Baldwin, director of the CDC’s Division of Unintentional Injury Prevention at the National Center for Injury Prevention and Control, set the stage for the panel discussion during the 7th ICF/George Washington University Annual Research and Evaluation Forum, Opioid Use: An Epidemic of Addiction, Not Abuse. He was joined by Capt. Jennifer Fan, Public Health Advisor at the Substance Abuse and Mental Health Services Administration (SAMHSA), and Gary Mendell, chairman and chief executive officer of advocacy group Shatterproof.
The panel, moderated by Dr. Lynn Goldman, the Michael and Lori Milken Dean of Public Health for the Milken Institute School of Public Health at George Washington University, focused on the complexities of the opioid epidemic and the various approaches to treatment, prevention and policy.
In the early days, there was an underappreciation for the addictive potential of opioids, combined with aggressive marketing of these drugs to clinicians, said Baldwin.
Prescription rates for opioids have since leveled off throughout much of the country, but the trend changed the way we, as a nation, approached pain management. It also laid the groundwork for the next two waves of the epidemic, characterized by more potent, deadly, and illicit opioids like heroin and fentanyl.
Ending the shame and stigma of addiction
Captain Fan noted that “stigma is one of the biggest hurdles to overcome” People impacted by substance use disorders are often embarrassed to tell friends or family that they or their loved ones are struggling. But having access to accurate information can help, as can opening the dialogue about addiction as a chronic disease that can be treated.
Powerful message to end the shame and stigma around #opioidepidemic @gary_mendell @ICFhealth #ICFGWforum @GWpublichealth pic.twitter.com/YMtedmq7Xn
— GWEpiontheRun (@GWEpiontheRun) November 1, 2017
CDC is looking to further the national conversation on addiction, and recently launched Rx Awareness, a communications campaign that emphasizes the near-immediate impact of these powerful drugs: “It only takes a little to lose a lot,” reads the campaign’s tagline. The campaign focuses on reaching people with resources and personal stories of addiction in Kentucky, New Mexico, Ohio, and West Virginia--four states that have been hit especially hard by the opioid epidemic.
We need the worforce moving forward to help with this epidemic, according to Dr. Grant Baldwin, from the CDC @ the ICF/GW Forum #ICFGWForum pic.twitter.com/apL6rRAU57
— Pam Jeffries (@GWDeanJeffries) November 1, 2017
That’s only the first step. Ultimately, the goal is to harness research, resources, and the voices of those affected to advocate for change. That’s what happened with conditions like breast cancer, autism and HIV/AIDS, all of which were highly stigmatized in the past. As people started to speak up and speak out about these diseases, others who were previously ashamed to share their diagnoses (or those of family members and friends) found comfort and empowerment. And with more support from individuals and organizations comes more opportunities for research and policy change at all levels of government.
The best treatment is prevention
To effectively mitigate the opioid epidemic, federal agencies must take two-pronged approach: preventing future addiction and treating people who are already addicted. It requires a collaborative effort among all federal agencies as well as external stakeholders. Already, CDC and SAMHSA are developing a joint campaign that addresses the knowledge gap around opioid use and answers some of the pressing questions among patients, practitioners, and caregivers, including:
- What are the consequences of prescribing opioids for pain?
- What should patients know when they are prescribed?
- Where are the existing gaps, and how can community stakeholders combat the issue?
From a healthcare perspective, developing a national standard of care in collaboration with insurers has been a top priority for Mendell’s organization. Shatterproof analyzed 60 evidence-based protocols and processes that improve patient outcomes, and came up with eight principles of care for addiction treatment. The organization plans to also develop an infrastructure to measure and reward the providers who follow these standards.
“These are not bad people doing bad things,” said Mendell. “These are good people with a serious disease.”
Will new prevention and treatment methods enable us to effectively combat the opioid epidemic? Let us know your thoughts on LinkedIn, Facebook or Twitter using #ICFGWForum.
